I remember using a ton of eye drops and never getting any relief. I was finding pieces of Sclera (the white, dense, fibrous outer coating of the eyeball) inside the lids and I was getting scarring. I was working full time and going to school at night; looking at a computer screen all day and books all night made it much worse! The lights at night were a big blur and I couldn’t focus at all. My eyes were literally drying up. I was having ongoing eye infections. To say the least I was going blind and was petrified. I couldn’t wear contacts to save my life. They would pop right out or worse, get caught in the corner of my eye.
I saw an eye doctor who never gave me answers. He never thought to test me for Sjögren’s Syndrome. They put silicone plugs in my tear ducts to try and keep what little moisture I had in my eyes. Talk about a scary situation! My general doctor was determined to find out what was going on because it went way beyond the eyes. I was extremely fatigued and had major joint and muscle pain, stomach issues, brain fog and upper respiratory infections often. I was pretty discouraged, but felt lucky my doctor cared, who by the way told me it wasn’t in my head (nice rarity). I knew eventually we would figure it out. He ran some blood work and pulled out the big guns (gigantic reference book) while explaining I had Sjögren’s Syndrome and sent me to a Rheumatologist. I was not in the mood to add more medication to my already long list at the time and decided to look into alternative care. I already had developed hypothyroid – another autoimmune disease. Since going gluten, dairy and soy free, I have been able to wear contacts daily and most of the symptoms from Sjögren’s are gone. I consider myself one of the lucky ones who took control and is able to manage a great deal with nutrition alone.
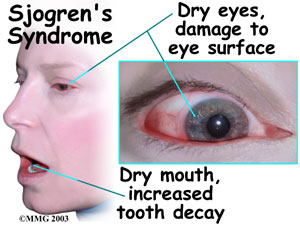
What is Sjögren’s
Sjögren’s syndrome is a chronic autoimmune disease in which people’s white blood cells attack their moisture-producing glands. Today, as many as four million Americans are living with this disease.
Although the hallmark symptoms are dry eyes and dry mouth, Sjögren’s may also cause dysfunction of other organs such as the kidneys, gastrointestinal system, blood vessels, lungs, liver, pancreas, and the central nervous system. Patients may also experience extreme fatigue and joint pain and have a higher risk of developing lymphoma.
With upwards of 4,000,000 Americans suffering from Sjögren’s syndrome, it is one of the most prevalent autoimmune disorders. Nine out of 10 patients are women. About half of the time Sjögren’s syndrome occurs alone, and the other half it occurs in the presence of another autoimmune connective tissue disease such as rheumatoid arthritis, lupus, or scleroderma. When Sjögren’s occurs alone, it is referred to as “Primary Sjögren’s.” When it occurs with another connective tissue disease, it is referred to as “Secondary Sjögren’s.”
All instances of Sjögren’s syndrome are systemic, affecting the entire body. Symptoms may remain steady, worsen, or, uncommonly, go into remission. While some people experience mild discomfort, others suffer debilitating symptoms that greatly impair their functioning. Early diagnosis and proper treatment are important – they may prevent serious complications and greatly improve a patient’s quality of life.
Since symptoms of Sjögren’s syndrome mimic other conditions and diseases, Sjögren’s can often be overlooked or misdiagnosed. On average, it takes nearly seven years to receive a diagnosis of Sjögren’s syndrome. Patients need to remember to be pro-active in talking with their physicians and dentists about their symptoms and potential treatment options.
Testing
There is no single test that will confirm diagnosis. Rheumatologists have primary responsibility for diagnosing and managing Sjögren’s syndrome and can conduct a series of tests and ask about symptoms. An international group of experts formulated classification criteria for Sjögren’s syndrome which help doctors arrive at a diagnosis. These criteria consider dryness symptoms, changes in salivary (mouth) and lacrimal (eye) gland function, and systemic (whole body) findings.
Blood tests your physician may perform include:
ANA (Anti-Nuclear Antibody)
ANAs are a group of antibodies that react against normal components of a cell nucleus. About 70% of Sjögren’s patients have a positive ANA test result.
RF (Rheumatoid Factor)
This antibody test is indicative of a most often performed for the diagnosis of rheumatoid arthritis (RA) but is positive in many rheumatic diseases. In Sjögren’s patients, 60-70% have a positive RF.
SS-A (or Ro) and SS-B (or La)
These are the marker antibodies for Sjögren’s. Seventy percent of Sjögren’s patients are positive for SS-A and 40% are positive for SS-B (these may also found in lupus patients).
ESR (Erythrocyte Sedimentation Rate)
This test measures inflammation. An elevated ESR indicates the presence of an inflammatory disorder, including Sjögren’s syndrome.
IGs (Immunoglobulin’s)
These are normal blood proteins that participate in immune reactions and are usually elevated in Sjögren’s patients.
The ophthalmologic (eye) tests include:
Schirmer Test
Measures tear production.
Rose Bengal and Lissamine Green
Eye drops containing dyes that an eye care specialist uses to examine the surface of the eye for dry spots.
The dental tests include:
Salivary Flow
Measures the amount of saliva produced over a certain period of time.
Salivary scintigraphy
A nuclear medicine test that measures salivary gland function.
Salivary gland biopsy (usually in the lower lip)
Confirms inflammatory cell (lymphocytic) infiltration of the minor salivary glands.
Your physician will consider the results of these tests along with your physical examination to arrive at a final diagnosis. Further research is being conducted to refine the diagnostic criteria for Sjögren’s syndrome and to help make diagnosis easier and more accurate.
Treatments
The treatment of patients with Sjogren’s syndrome is directed toward the particular areas of the body that are involved and complications, such as infection. There is no cure for Sjogren’s syndrome.
Dryness of the eyes can be helped by artificial tears, eye-lubricant ointments at night, and minimizing the use of hair dryers. When dryness becomes more significant, the ophthalmologist can plug the tear duct closed so that tears cover the eye longer. Cyclosporine eye drops (Restasis) are recently approved medicated drops that can reduce the inflammation of the tear glands improving their function. These however are painful to use and have side effects. Signs of eye infection (conjunctivitis), such as pus or excessive redness or pain, should be evaluated by the doctor.
The dry mouth can be helped by drinking plenty of fluids, humidifying air, and good dental care to avoid dental decay. The glands can be stimulated to produce saliva by sucking on sugarless lemon drops or glycerin swabs. Artificial saliva preparations can ease many of the problems associated with dry mouth. Many of these types of agents are available as over-the-counter products, including toothpaste, gum, and mouthwash (Biotene). Vitamin E oil has been used with some success. Infections of the mouth and teeth should be addressed as early as possible in order to avoid more severe complications. Diligent dental care is very important. Saltwater (saline) nasal sprays can help dryness in the passages of the nose. Vaginal lubricant should be considered for sexual intercourse.
As mentioned, each person is different in how they are affected by Sjögren’s. Because I know first hand I would say first and foremost – GO OFF GLUTEN. Once you have that under control you can talk to your doctors about complimentary treatments if needed. The biggest thing with any auto immune disease is inflammation. Make that your number one goal to have that under control. Consider a holistic approach which has no side effects and is a lot safer.
Some essential survival tips for Sjögren’s patients:
- Avoid stomach upset.
- Never feel guilty about seeking a second opinion.
- Join a support group if needed.
- Listen to your body. Do not take on more than you can handle, and pay attention to new symptoms, or symptoms that get worse, and tell your practitioner.
- Do your research.
- Make sure you coordinate all of your care in Sjögren’s and head your “medical care team.” You want to make sure you are keeping records on medications, supplements and herbs. Make sure your physician knows about all the prescription and OTC medications you are taking. Many drugs have side effects that can make your Sjögren’s symptoms worse.
- Become an active participant in your treatment decisions and an informed consumer. You will feel more in control of your disease, decrease anxiety, and ensure you are getting the best possible medical care for you.
- You can maintain a good quality of life with Sjögren’s. Stay on top of the latest information, educate yourself, find support and watch your limits.
- Keep positive relationships and support in your life. These will help you cope and will reduce general anxiety when you have a frequently misunderstood disease.
Dry Mouth Survival Tips
- Eat soft, moist foods if you have trouble swallowing or with your teeth chipping and breaking.
- Sjögren’s patients should eat smaller, more frequent meals to stimulate saliva flow.
- Avoid salty, acidic or spicy foods and carbonated drinks that may be painful on your dry mouth or interfere with digestion in Sjögren’s.
- Help prevent dental decay by using oral products containing the sweetener xylitol For dry mouth, increase your intake of liquids during the day. Remember that small sips of water work best.
- Sjögren’s patients should avoid mouthwashes and rinses that contain alcohol or witch hazel. These ingredients can aggravate oral dryness and burning.
- Chew sugar-free gum or suck on hard diabetic or sugar-free candies to help increase saliva. The best gum I’ve found has xylotil called Spry. They also carry mints.
- Apply vitamin E oil or moisturizing gels to dry or sore parts of the mouth or tongue for long-lasting relief. Use the liquid oil or punch holes in vitamin capsules to apply.
Dry Eye Survival Tips
- Try sterile eyelid cleansers or baby shampoo on a warm washcloth to help with blepharitis, a common condition in Sjögren’s that causes chronic inflammation of the eyelids and eyelid margins.
- For dry eye, apply a warm, wet compress to the closed eyes using a washcloth. Apply at bedtime and upon awakening for 5 minutes, or more often if helpful.
- The mainstay of treatment for blepharitis, a chronic condition that accompanies dry eye and Sjögren’s, is warm compresses, lid massage and lid hygiene.
- If your eyes are bothered by light, wear sunglasses or try lenses with a FL-41 filter.
- Avoid applying anything to the eyelids that can irritate your dry eye; products placed on the eyelid will get into the tear film.
- Use non-preserved artificial tears frequently and regularly, even when your eyes feel good. The goal is to keep your eyes comfortable, not to wait until they are uncomfortable.
- Keep the upper and lower eyelids free of facial creams at bedtime; they can enter the eye and cause irritation.
- Try ointments or gels at bedtime by first applying them only to the eyelids and lashes. If that is not helpful, place ~1/4 inch of ointment between the lower lid and eyeball.
- Eye ointments and gels can blur your vision and are usually reserved for overnight use.
- If your vision is blurred with artificial tear use, try a less thick (viscous) drop or ointment.
- Try moisture chamber glasses, wrap-around sunglasses, or other glasses, goggles or shields to prevent moisture evaporation and offer protection from air currents that irritate your dry eye.
Dry Skin Survival Tips
- Take short, warm baths or showers to help with dry skin. Hot water removes skin oils.
- Sjögren’s patients with dry skin should pat dry after bathing and moisturize immediately while the skin is still damp. Natural oils such as coconut, almond, sesame and apricot work well.
- Sjögren’s patients with dry and/or sensitive skin should avoid fabric softeners in the washer and dryer. Always use hypoallergenic products.
- After swimming, make sure that you shower and immediately use a moisturizer to reduce dry skin symptoms.
Sun & Sjögren’s Survival Tips
- To reduce reactions to the sun, wear good UV-protective eye lenses and sunglasses, and seek the shade when outside.
- Protect your skin and eyes through use of sunscreen, sunglasses, ultraviolet light-protective clothing, hats, and non-fluorescent lighting.
- Did you know that ultraviolet (UV) radiation from the sun and other light sources can affect Sjögren’s patients, leading to skin rashes, disease flares, eye sensitivity and pain?
- Consider purchasing UV-protective car and home window films that are clear or tinted to protect yourself from UV radiation.
- Look for the words “broad spectrum” on sunscreen protection. This means that you will be protected from both UVA and UVB radiation.
- Make sure you are taking enough Vitamin D3 and antioxidants.
Fatigue Survival Tips
- Battling fatigue with Sjögren’s? Know your limits and pace yourself.
- Don’t be a couch potato! A common cause of chronic pain and fatigue in any disorder, including Sjögren’s syndrome, is lack of exercise.
- Educate your friends and family about what you are going through and how fatigue in Sjögren’s syndrome can come and go.
- Sjögren’s can cause fatigue, but there can be other related causes such as adrenal fatigue or hypothyroid disease and depression.
Brain Fog Survival Tips
- Did you know that “brain fog” is a major complaint of Sjögren’s patients? Hint: Train the brain! If you don’t use it, you will lose it.
- Don’t assume your “brain fog” is due to Sjögren’s, especially in patients over 65-70 years of age: a major cause of cognitive dysfunction can be side effects of drugs and drug interactions and food intolerance such as gluten and dairy. These foods are inflammatory and cause an opiate affect similar to brain fog.
- To help symptoms of “brain fog,” minimize stress and anxiety. Take breaks throughout the day and learn relaxation exercises and practice them at regular intervals.
- Reduce caffeine and alcohol to help with “brain fog” and sleep problems in Sjögren’s.
Dry Nose & Sjögren’s Survival Tips
- Use natural saline spray several times a day if needed. Clean and moisture nasal cavity in the morning and again at night. This helps keep allergens from settling in the cavity as well.
- Dry Ear Survival Tips
- A drop of earwax remover or mineral oil can help dry itching ears.
Herbal Remedies and Supplements
Rosemary
The rosemary plant contains several anti-inflammatory agents that help in the prevention of arthritic pain and dryness caused by Sjogren’s Syndrome. It is recommended to make rosemary tea instead of eating the plant. Mix a half an ounce of rosemary leaves in a pot of boiling water. Cover the pot, and let the mixture simmer for 30 minutes. Consume the tea before going to bed. This can be repeated as often as necessary.
Evening Primrose Oil
Evening primrose oil contains gamma linolenic acid, also known as GLA. GLA is a fatty acid that helps Sjogren’s Syndrome sufferers by introducing prostaglandin into the system. Prostaglandin in turn works as an anti-inflammatory to help common Sjogren’s Syndrome symptoms. Evening primrose oil should be taken daily, with a dosage of 3,000- to 6,000-mg.
Celery Seeds
Celery contains several different anti-inflammatory agents that can help Sjorgren’s Syndrome symptoms such as joint paint, inflammation, and lethargy. Celery also packs over 340 milligrams of potassium per single cup. This is beneficial to anyone with an autoimmune disease, since lack of potassium can cause arthritic like symptoms. Celery plants can be eaten in large quantities, but for faster and easier results, celery seeds are recommended. Place a teaspoon of celery in a cup of boiling water. Up to three cups daily may be consumed.
Gamma-linolenic acid (GLA) may actually reduce inflammation. Much of the GLA taken as a supplement is converted to a substance called DGLA that fights inflammation. Having enough of certain nutrients in the body (including magnesium, zinc, and vitamins C, B3, and B6) helps promote the conversion of GLA to DGLA.
Cysteine is an amino acid that can be found in many proteins throughout the body. When used as a supplement, it is usually in the form of N-acetyl-L-cysteine (NAC). The body converts this to cysteine and then to glutathione, a powerful antioxidant reducing symptoms associated with Sjögren’s syndrome.
REFERENCES:
Koopman, William, et al., eds. Clinical Primer of Rheumatology. Philadelphia: Lippincott Williams & Wilkins, 2003.
Kelley’s Textbook of Rheumatology, W B Saunders Co, edited by Shaun Ruddy, et al., 2000.
Sjögren’s Foundaton.
You can read all about Sandi Star’s remarkable story in her 3-part article series available at the following links: Living Gluten Free – Right to Heal – Part I, Living Healthy, Without Gluten and Dairy– Part II, Living Healthy, Without Gluten and Dairy Part III.
About the author: Sandi Star, CCN Sandi is the founder of Karmic Health, specializing in nutrition related to disease where a gluten and casein (dairy) free lifestyle is crucial; working with celiac, autism and all auto immune disorders. Sandi graduated from The Natural Healing Institute with a degree in Clinical Nutrition and is continuing her studies in Clinical Herbology. She has hands on understanding of many health issues and has dedicated her life in helping others reach their optimal health.
For more information related to this article (or her previous articles) please visit www.karmic-health.com or contact Sandi Star at 760.685.3154.
Tina Turbin
www.GlutenFreeHelp.info